Click here to read the July 29 newsletter.
 “Bernhardt Wichmann III in his room in Manhattan in 2009. ‘He had plenty of reasons to be unhappy,’ a friend said. ‘But I never saw him unhappy.’” Credit Ángel Franco/The New York Times
“Bernhardt Wichmann III in his room in Manhattan in 2009. ‘He had plenty of reasons to be unhappy,’ a friend said. ‘But I never saw him unhappy.’” Credit Ángel Franco/The New York Times
This is a wonderful story of a man who embodied “happy.”
by N.R. Kleinfeld | The New York Times
“The man who lost his voice was a gentle man who didn’t ask terribly much of life. He lived in a miniature space in a single-room-occupancy residence on the corner of 74th Street and Third Avenue in Manhattan, above J. G. Melon, the popular restaurant and bar known for succulent hamburgers. And he was a New York story.
“He was a New York story because he didn’t have a lot and yet he gave a lot. And in return he got what New York for all its busyness so often offers those who could use a good dose of it — kindness. The city can be cold and aloof and you can live crunched amid its population and remain lonely and overlooked. You can also be someone unremarkable and be made to feel like Mr. Big Shot.
“The name of the man who lost his voice was Bernhardt Wichmann III. Sounds like an old-money name for sure, but any money ever attached to it was no longer visible.”
Read this article about Mr. Wichmann in its entirety at The New York Times.
Click here to read the July 29 newsletter.
Today Pennlive, The Patriot-News (Harrisburg, PA) Website, posted a slideshow about Medicare’s “Star Rating” Hospital Compare showing a glimpse of ratings for mid-state hospitals.
“The Centers for Medicare & Medicaid Services (CMS), along with key stakeholders, developed (the star rating) methodology to calculate and display overall hospital-level quality using a star rating system.
“The overarching goal of the Overall Hospital Quality Star Rating is to improve the usability and interpretability of information posted on Hospital Compare, a website designed for consumers to use along with their healthcare provider to make decisions on where to receive care. CMS developed this methodology with the input of a broad array of stakeholders to summarize results of many measures currently posted on Hospital Compare. The Overall Hospital Quality Star Rating provides consumers with a simple overall rating generated by combining multiple dimensions of quality into a single summary score.” - QualityNet.org
Customers can access the Medicare Hospital Compare screen here.
“Choosing a hospital is a complex and personal decision that reflects individual needs and preferences. You should consider a variety of factors when choosing a hospital, such as physician guidance about your care plan and other sources of information about hospitals in your area.” - Medicare.gov
Two more articles you may want to read:

By Jennifer L. Boen | (This article appeared previously in the Fort Wayne News-Sentinel/New America Media.)
“Rozanne and Gerald Hallman were thrust unexpectedly and severely into the land of the seriously ill when, in late 2011, Gerald, a retired pastor, was diagnosed with a brain tumor. He underwent surgery to remove as much tumor as possible, but the procedure left him paralyzed on one side.
“‘They said [his tumor] was a bad one,’ Rozanne recalled. Many questions and decisions faced the rural Steuben County, Ind., couple.
“When Gerald’s physicians discussed options and next steps, palliative care was among them. Rozanne, a retired teacher, was familiar with hospice, but unaware of palliative care as a specialized service that helps improve quality of life without necessarily abandoning curative treatment.
“In medical school, the very little I got about suffering and death ill-prepared me for what I would encounter.” — Dr. Andrew Esch, Center to Advance Palliative Care
“‘I didn’t have a clue,’ she said, but added that through those services, ‘our every need was met.’
“Multiple studies show that, compared to awareness of hospice, “There’s significantly less familiarity with palliative care,” said Dr. Lyle Fettig, director of Indiana University School of Medicine’s Hospice and Palliative Medicine Fellowship program centered in Indianapolis.”
Read this article in its entirety at nextavenue.com.
“Medical faculties have traditionally eschewed teaching the subject, in part because many physicians viewed addiction as a personal vice rather than a disease.”
 Between 1999 and 2014, the number of deaths in the U.S. from prescribed opioids quadrupled. Meanwhile medical students were getting very little training on how to spot patients who are at risk for addiction, or how to treat it. - Matt Lincol/Getty Images/Cultura Exclusive
Between 1999 and 2014, the number of deaths in the U.S. from prescribed opioids quadrupled. Meanwhile medical students were getting very little training on how to spot patients who are at risk for addiction, or how to treat it. - Matt Lincol/Getty Images/Cultura Exclusive
by Natalie Jacewicz | NPR
“Jonathan Goodman can recall most of the lectures he’s attended at the Stanford University School of Medicine. He can recite detailed instructions given more than a year ago about how to conduct a physical.
“But at the end of his second year, the 27-year-old M.D.-Ph.D. student could not remember any class dedicated to addiction medicine. Then he recalled skipping class months earlier. Reviewing his syllabus, he realized he had missed the sole lecture dedicated to that topic.
“‘I wasn’t tested on it,’ Goodman says, with a note of surprise.
“Americans are overdosing on opioids such as heroin and prescribed painkillers at epidemic rates, and the nation’s doctors appear to be inadequately prepared to help.
“The problem begins in medical school.”
HARRISBURG (July 26, 2016) – Auditor General Eugene DePasquale said today that his audit of the Department of Health’s (DOH) oversight of nursing homes has already led to changes that should improve the quality of care residents receive.

“The quality of care provided to 80,000 Pennsylvanians who live in nursing homes is directly related to adequate staffing,” DePasquale said in announcing the 91-page audit, which has 13 findings — more than any special performance audit since he took office — and 23 recommendations. “The Department of Health has work to do in making sure these facilities are appropriately staffed.
“Assuring adequate nursing staff are on duty at all times, investigating all complaints — including those submitted anonymously — in a timely manner and imposing monetary sanctions when necessary are three key functions of DOH’s oversight of nursing homes,” DePasquale continued. “Implementing this audit’s recommendations will be crucial to improving the care that residents receive.”
DePasquale commended DOH for taking a proactive stance to improve its operations.
Click here to read the press release from the Auditor General’s Website in its entirety.
“Suicide is the third leading cause of death among young people. In Allegheny County (Pa.), several efforts are ongoing to stem the loss of life through suicide prevention tools.”
by Mary Niederberger | PublicSource
 Illustration by Anita DuFalla | Public Source
Illustration by Anita DuFalla | Public Source
“It is a group of 108 that includes middle and high school athletes and artists, fraternity and sorority members, folks who loved to fish, hunt and work on cars, some wayward teens, some students pursuing math and science degrees, a rookie police officer and others in fledgling careers.
“They were siblings, children, grandchildren and, in some cases, parents.
“Their ages range from 13 to 24.
“They came from all corners of Allegheny County and a few outliers.
“They are the young people who passed through the Allegheny County Medical Examiner’s office between Jan. 1, 2011, and July 11, 2016, because they took their own lives.
“They leave behind 108 versions of the question: Why?”
Read this gripping article at Public Source; click here.
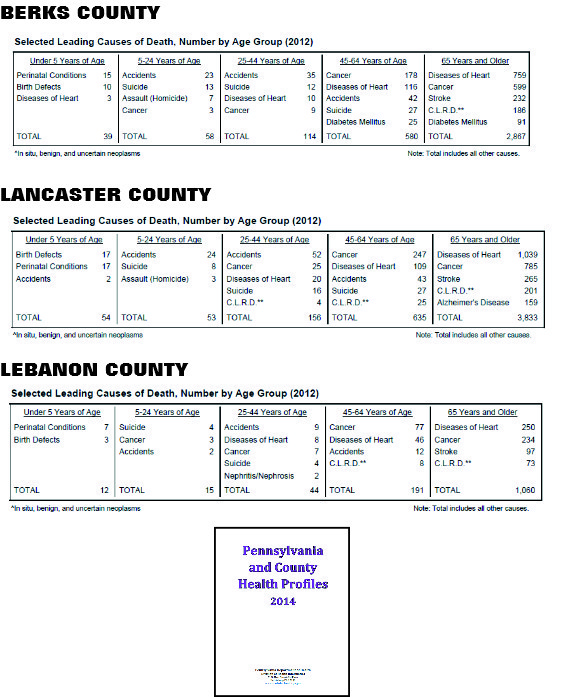 Suicide is first or second among the younger demographics in the Pennsylvania Link to Aging and Disability Resources’ Berks-Lancaster-Lebanon Service Area too according to the among the Pennsylvania County Health Profiles - 2014 Report.
Suicide is first or second among the younger demographics in the Pennsylvania Link to Aging and Disability Resources’ Berks-Lancaster-Lebanon Service Area too according to the among the Pennsylvania County Health Profiles - 2014 Report.

Each week the Office of the Secretary of Pennsylvania’s Department of Aging releases a Friday newsletter with information relevant to activities, issues and events for older Pennsylvanians and persons with disabilities across the Commonwealth.
Click here to read the July 22 newsletter.
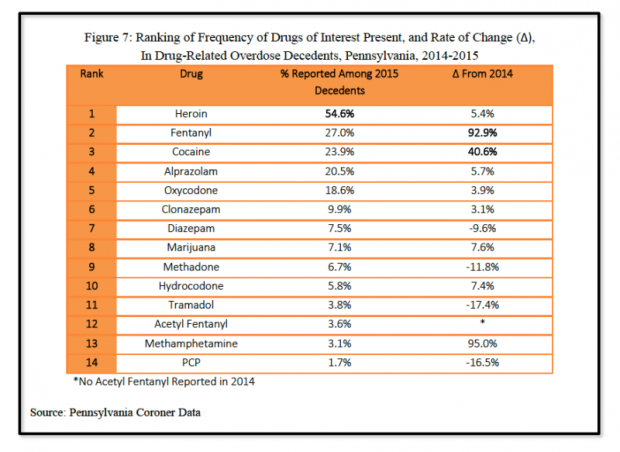
By Jeffrey Benzing | PublicSource
“The federal government has grim news on overdose deaths in Pennsylvania.
“Already in the midst of a drug crisis that kills more people statewide than car crashes, overdose deaths spiked nearly 25 percent last year, according to the Drug Enforcement Administration’s Philadelphia Field Division.
“By the agency’s count, 3,383 Pennsylvanians died in drug-related overdoses in 2015. Heroin or opioid painkillers were found in 81 percent of cases, the report said.
“Heroin itself was found in more than half of all cases. Fentanyl, a powerful painkiller, is the second most common drug detected. Its popularity has soared, and it was detected in more than a quarter of cases, up nearly 93 percent from 2014.”