Each week the Office of the Secretary of Pennsylvania’s Department of Aging releases a Friday newsletter with information relevant to activities, issues and events for older Pennsylvanians and persons with disabilities across the Commonwealth.Click here to read the August 26 newsletter.
“Build the foundation to be a CCBHC, make sure you are trauma-informed” - National Council for Behavioral Health
This email message from the National Council for Behavioral Health is too important to not share.

Are you embracing the urgency to become trauma-informed? Certified Community Behavioral Health Clinics (CCBHC) are poised to revolutionize behavioral health care and strengthen services for those who most need them. Organizations are preparing to meet CCBHC requirements in the areas of finance, service delivery and partner collaboration.
CCBHCs aren’t business as usual. They’re a new provider type in Medicaid— organizations defined not just by the comprehensive array of services they provide, but by their focus on trauma-informed care, recovery and wellness. That means trauma isn’t just one more box to check to meet CCBHC requirements: it’s a foundation for all the work a CCBHC does.
 Click on this graphic to connect to Pennsylvania’s CCBHC page at the Department of Human Services Website.
Click on this graphic to connect to Pennsylvania’s CCBHC page at the Department of Human Services Website.Consider some of the CCBHC requirements related to trauma-informed care:
- CCBHC staffing must include, “individuals with expertise in addressing trauma and promoting the recovery” of both children and adults.
- CCBHCs must regularly provide staff with training about evidence-based and trauma-informed care.
- When conducting client evaluations, CCBHCs are encouraged to screen for behavioral health history, including trauma history.
To meet these criteria, organizations must consider a number of organizational changes: hiring practices that seek to recruit and retain staff with trauma expertise; integration of a trauma focus into ongoing trainings for all staff; and provider-client interactions that begin with and are informed by an understanding of that client’s trauma history. At the end of the day, these changes ensure that CCBHCs will truly be trauma-informed organizations.
Why is it important?
Trauma is a near universal experience of individuals with behavioral health challenges. Unfortunately, trauma is too often shrouded in secrecy and its impact is often ignored and misunderstood. When we fail to ask about and address trauma and our services are not built on the emerging science around what trauma survivors need to heal and recover, we risk re-traumatizing the people we serve. Trauma-informed care is the path to ensuring we honor this most sacred promise, and offers great potential for effectively partnering with our clients to help them move forward in their recovery and wellness. The good news is that this model not only strengthens the individuals we serve, but our organizations overall. For example, a trauma-informed organization ensures that all staff, including your peer providers (a CCBHC staffing requirement), can work in a safe and secure environment that doesn’t re-traumatize them.
What does it mean to be trauma-informed?
According to SAMHSA—and reiterated in the CCBHC guidance-a trauma-informed approach reflects adherence to six key principles rather than a prescribed set of practices or procedures. These principles may be generalizable across multiple types of settings, although terminology and application may be setting- or sector-specific:
- Safety
- Trustworthiness and transparency
- Peer support
- Collaboration and mutuality
- Empowerment, voice and choice
- Cultural, historical, and gender issues
An organization that reflects these principles in all policies and procedures and every interaction with clients, staff, volunteers, board members and community partners, is well positioned to successfully meet the trauma-informed care requirements of a CCBHC.
What can organizations do to become trauma-informed?
National Council has a team of trauma experts – including Karen Johnson, Linda Henderson-Smith and Cheryl Sharp – who have helped hundreds of entities, spanning community behavioral health organizations, primary care clinics, government systems, schools, social services and law enforcement, develop and operationalize plans for becoming trauma-informed through training and consultation. Our experts are ready to help you infuse trauma-informed care into the foundation of your organization so you can rise to the challenge and embrace the promise of CCBHC innovation.
Ask how the National Council’s trauma-informed consulting can be tailored to meet the needs of your organization — contact Sharday Lewis at shardayl@thenationalcouncil.org.
“Retiring On Social Security Alone What’s it like to live on just social security?” - Grandparents.com

“Barbara Woodruff of St. Louis shares her story, and it may surprise you.”
“No doubt you’ve heard politicians and pundits debating the state of social security, and throwing out all kinds of numbers. But the bottom line for retirees has always been simple: Will I get enough to live on?
“Barbara Woodruff, of St. Louis, MO, can answer “yes,” to that question, but just barely. ‘It’s very difficult living on social security,’ says the 65-year old, who retired when she turned 62. Having lost her job as a cashier as well as her apartment and car in the recession, and being unable to find another job, the single retiree felt she had little choice but to retire in order to have an income. Her total social security benefit : $633 a month.
“According to the Social Security Administration, Woodruff is far from alone.”
Click here to read this article at Grandparents.com in its entirety.
Pennsylvania Announces Selection for Community HealthChoices Managed Care Agreements
The Department of Human Services (DHS) continues to improve access to high-quality services and serve more people in the community.
Harrisburg, PA – Today, the departments of Human Services (DHS) and Aging announced that the commonwealth has agreed to move forward and negotiate agreements with three managed care organizations (MCOs) for Community HealthChoices (CHC).
CHC will coordinate physical health and long-term services and supports (LTSS), if needed, to enhance the quality of medical care and access to all appropriate services to more than 420,000 individuals who are dually eligible for Medicare and Medicaid, older Pennsylvanians and individuals with disabilities.
“We are committed to increasing opportunities for older Pennsylvanians and individuals with physical disabilities to remain in their homes. CHC allows us to serve more people in communities rather than in facilities, giving them the opportunity to work, spend more time with their families, and experience an overall better quality of life,” said DHS Secretary Ted Dallas. “The MCOs selected today will provide a choice of health care and LTSS providers to everyone moving into CHC and allow them to receive the services they need in a coordinated manner.”
Through a request for proposals, DHS has selected the MCOs to proceed with negotiations to deliver services in Pennsylvania beginning in 2017. The following MCOs were selected for negotiations on a statewide basis:
- AmeriHealth Caritas
- Pennsylvania Health and Wellness (Centene)
- UPMC for You
“Like many states across the country, the opportunity for Pennsylvania to further strengthen the social safety net, which is anchored by Medicare and Medicaid, by transitioning to a managed long-term services and supports model takes a major step forward today via this announcement,” said Secretary of Aging Teresa Osborne. “Eligible older Pennsylvanians and persons with physical disabilities are relying upon the departments of Aging and Human Services to ensure that this transition is seamless, and our proceeding in dialogue with these managed care organizations demonstrates the Wolf Administration’s commitment to ensuring that Pennsylvanians can access necessary services and supports in order to age in place.”
The MCO agreements will also continue the departments’ increased focus on greater coordination between the physical and behavioral health systems, as well as LTSS. CHC will:
- Enhance opportunities for community-based services and increase access to services;
- Strengthen health care and LTSS delivery systems;
- Allow for new innovations;
- Promote the health, safety, and well-being of enrolled participants; and
- Ensure transparency, accountability, effectiveness, and efficiency of the program.
CHC will roll out in three phases. Persons eligible for CHC are 21 or older who have both Medicare and Medicaid, or who receive long-term services and supports through Medicaid because they need help with everyday activities of daily living.
The departments have created an overview of the program that can be seen here.
“At this community, residents blink to control just about everything” - Senior Housing News
 Steve Saling
Steve Saling
“At the Leonard Florence Center for Living, residents can control just about everything around them through a series of blinks.
“The community is located in Chelsea, Massachusetts and run by the Chelsea Jewish Foundation; it currently has 10 Green House-style skilled nursing residences with 10 bedrooms each. Two of the Green Houses are built for people living with amyotrophic lateral sclerosis (ALS), and one is specifically equipped for residents living with multiple sclerosis (MS).
“On these three floors, wheelchair-bound residents of all ages can control everything with an on-and-off switch—lights, televisions, window shades, air conditioning, phones—using only their eyes.
“The minds behind this innovative community believe its technology may have a future in more skilled nursing facilities, or even assisted living communities where seniors struggle with mobility.”
Read this article in its entirety at Senior Housing News, click here.
“Why We Never Die” - The New York Times | Opinion
 Andrea Fontanili/EyeEm, via Getty Images
Andrea Fontanili/EyeEm, via Getty Images
by Gabriel Rockhill | The Stone -A forum for contemporary philosophers and other thinkers on issues both timely and timeless.
“As a child, I was terrified of death. It was often in the twilight hours, between the moment of lying down and the imperceptible instant of slipping off to sleep, that the terror would arise. The thought of vanishing completely from the world, of being engulfed in ineradicable darkness, would seize upon me and crush with it the very existence of the world. It was not simply that I would no longer be there. It was that reality itself would collapse, devoid of any point of apprehension. Petrified before a void so vast that it could not be contained within thought, let alone a thinking being, it was impossible to know how long it would take to drift off into the abyss that silently beckoned me.
“Religion and spirituality were of little or no solace. Even to my young mind, they struck me as fantasies that had been elaborately constructed and forcefully imposed in order to stave off the horror. Their power paled in comparison with the groundless vacuum that they sought to mask, and my restless mind would have nothing of consolation. As I grew older, the appeal of philosophy was that it opened vantage points to stare into the vertiginous face of death, and to ponder the meaning of living in an uncertain world precariously perched on the absolute certainty of death.”
Click here to read this opinion piece in its entirety at The New York Times.
Want to engage in more discussing about death? Come to a free “Death Café.” Find out more here:
In Lancaster County on Saturday, September 10.
In Lebanon County on Tuesday, September 13.
“At a Death Cafe people drink tea, eat cake and discuss death. Our aim is to increase awareness of death to help people make the most of their (finite) lives” - DeathCafe.com
“The broken covenant | Behind the fragmented state of mental health care lies a political system failure that spans decades — and continues.” - The Boston Globe SPOTLIGHT TEAM
Today’s Boston Globe‘s SPOTLIGHT TEAM‘s got several articles that focus on mental health - specifically, the articles are about Massachusetts, but the stories can be applicable nationwide.
“Few have paid a higher price for the nation’s mental health crisis than the loved ones of severely mentally ill people. At least 17 parents with signs of mental illness allegedly killed their children from 2005 through 2015, while a similar number of children allegedly killed their parents. But the toll of violence reaches far beyond family. From 2005 through 2015, 10 percent of all homicides in Massachusetts in which a suspect is known were allegedly committed by people with a history of mental illness or clear symptoms. Many of those deaths might have been prevented had the killers received the mental health care they needed.”
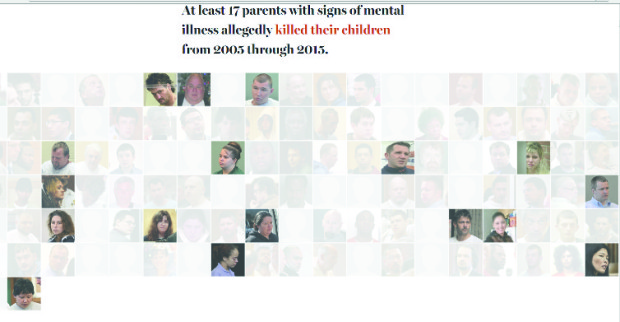 THE DESPERATE AND THE DEAD: FAMILIES IN FEAR
THE DESPERATE AND THE DEAD: FAMILIES IN FEAR



 “Hiroyuko Yamamoto, a crossing guard in Matsudo, Japan, has been trained in how to recognize and gently approach people who are wandering, or have other signs of dementia, in ways that won’t frighten them.” -
“Hiroyuko Yamamoto, a crossing guard in Matsudo, Japan, has been trained in how to recognize and gently approach people who are wandering, or have other signs of dementia, in ways that won’t frighten them.” -