“The Invisibility of Being Old, Disabled or Both | An 82-year-old woman with post-polio syndrome feels erased from society” - Next Avenue
 Photo source: next avenue - Credit: Adobe Stock
Photo source: next avenue - Credit: Adobe Stock
by Grace Bernstengel
“When you’re an older person in a wheelchair or walking with a cane, people treat you differently. Sure, some might be quicker to open doors for you, but most of the behavioral reactions aren’t positive ones. The combination of being old and disabled causes what many refer to as “invisibility.”
“Frank Bruni, an op-ed columnist for The New York Times, explored this idea in a recent column through the lens of 82-year-old Nancy Root, a woman with post-polio syndrome Bruni met while giving a lecture on a cruise. Root taught Bruni how it felt to be seen as invisible because of her age and perceived ability.
“‘People looked over her, around her, through her. They withdrew,’ Bruni wrote.
An intersection of -Isms
“The concept of invisible older people — specifically older women — is not new. Novelist and screenwriter Ayelet Waldman discussed with us the invisibility of turning 50 as a woman.
“’I had no idea that as soon as I got to his age, to be a 50-year-old woman, the sexism gets completely complicated by this idea that not only are you incompetent as a woman, but you’re incompetent because you’ve reached your senescence! Or something,’ Waldman told Next Avenue. ‘I really do feel like they don’t even see you.’”
Click here to continue reading this next avenue article in its entirety.
Attendant Care / Act 150
If you have a physical disability, the Attendant Care Waiver and state funded Act 150 program may be available to you to continue to live in your home and community with support and services.
 To download the above graphic as a .pdf format for enlarging, printing or sharing, click on the graphic or here: Act 150.
To download the above graphic as a .pdf format for enlarging, printing or sharing, click on the graphic or here: Act 150.
LEARN MORE HERE | Eligibility details, application forms and other information are available here.
Online training opportunities for Community Health Choices.
Though the implementation of Community Health Choices (CHC) is just over two years away for Berks, Lancaster and Lebanon Counties, on January 1, 2018, CHC begins in Southwestern Pennsylvania.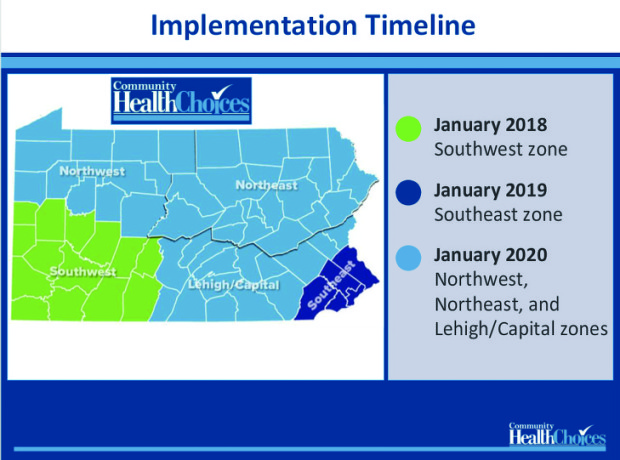
Community HealthChoices will deliver long-term services and supports and physical health benefits through capitated Medicaid managed care organizations (MCO). The CHC-MCOs will coordinate with Medicare and existing behavioral health HealthChoices MCOs to provide a holistic approach to services and supports. In order to transition to CHC, providers will enter into an agreement with a CHC-MCO and will be included in that CHC-MCO’s provider network. For a minimum of the first six months of the implementation of CHC, CHC-MCOs will be required to include all willing long-term services and supports providers in their network to ensure continuity of care for participants.
Prior to implementation and during the six-month period, CHC-MCOs will contract with willing and qualified providers of all types to make up their provider networks. CHC-MCOs are required to create a provider network that meets the needs of their participants and allows participants to have choice in providers.
Providers will also receive direct communications to inform them of actions that they need to take in order to continue providing services under this new model.
Training
Service Coordinators
- For the general public - Service Coordination Online Course
- For service coordinators only, visit the following website for instructions on how to complete the training which includes a test to verify competency.
Nursing Facilities
- For the general public - Nursing Facility Training
- For nursing facilities only, visit the following website for instructions on how to complete the training.
- Nursing Facility Eligibility & Enrollment Webinar
Additionally, there is helpful information at the Third Thursday Webinar series
“‘Crisis mode’: As boomers age, a shortage of caregivers” - The Baltimore Sun
 “Open Arms Solutions caregiver Kamlesh Debi, left, brings a slice of pie to Frank Shapira, 91, right, Monday, Nov. 20, 2017 at Shapira’s Skokie apartment, where he receives 24-hour home health care.” (Chris Walker / Chicago Tribune)”
“Open Arms Solutions caregiver Kamlesh Debi, left, brings a slice of pie to Frank Shapira, 91, right, Monday, Nov. 20, 2017 at Shapira’s Skokie apartment, where he receives 24-hour home health care.” (Chris Walker / Chicago Tribune)”
by Robert Channick, Contact Reporter Chicago Tribune
“As more and more baby boomers cross the threshold into old age, members of the Me Generation are confronting a growing problem: Who will take care of them when they can no longer care for themselves?
“It’s a situation few families are prepared for, but one many will face. As relatives gather for the holidays, it often becomes clear that falls, memory lapses and an assortment of maladies have taken a toll on aging loved ones and help is needed.
“But a shortage of qualified workers, rising costs and a massive demographic shift have newly minted seniors facing a caregiver crisis that could take some of the luster out of their golden years.”
Read this article in its entirety, click here.
PA Higher Education Consortium’s 2018 Symposium at Hershey Lodge

While most are counting down for the New Year, we invite you to countdown with us the days until Symposium 2018 - The Journey of Inclusion: Experiencing the College Years.
… for more information and details about the day with our Award-Winning Authors, International Leaders and Innovators - John O’Brien, Bruce Uditsky, and Cate Weir.
Scholarship Available
If you are interested in applying for a scholarship to attend the Symposium please see the application below:
“How Social Isolation Is Killing Us” - The New York Times
 “Social isolation is a growing epidemic, one that’s increasingly recognized as having dire physical, mental and emotional consequences. | Credit Damon Winter/The New York Times”
“Social isolation is a growing epidemic, one that’s increasingly recognized as having dire physical, mental and emotional consequences. | Credit Damon Winter/The New York Times”
by
“My patient and I both knew he was dying.
“Not the long kind of dying that stretches on for months or years. He would die today. Maybe tomorrow. And if not tomorrow, the next day. Was there someone I should call? Someone he wanted to see?
“Not a one, he told me. No immediate family. No close friends. He had a niece down South, maybe, but they hadn’t spoken in years.
“For me, the sadness of his death was surpassed only by the sadness of his solitude. I wondered whether his isolation was a driving force of his premature death, not just an unhappy circumstance.
“Every day I see variations at both the beginning and end of life: a young man abandoned by friends as he struggles with opioid addiction; an older woman getting by on tea and toast, living in filth, no longer able to clean her cluttered apartment. In these moments, it seems the only thing worse than suffering a serious illness is suffering it alone.”
Click here to read this New York Times article in its entirety.
“A Better Kind of Nursing Home” - The New York Times
 “The Green Houses at Green Hill continuing care facility in West Orange, N.J., offer residents greater autonomy and a homier, less hospital-like environment than at most nursing homes. Credit Bryan Anselm for The New York Times”
“The Green Houses at Green Hill continuing care facility in West Orange, N.J., offer residents greater autonomy and a homier, less hospital-like environment than at most nursing homes. Credit Bryan Anselm for The New York Times”
by Paula Spahn
“Lots of things look different when you step into a small Green House nursing home.
“The bright living and dining space, filled with holiday baubles at this season. The adjacent open kitchen, where the staff is making lunch. The private bedrooms and baths. The lack of long stark corridors, medication carts and other reminders of hospital wards.
“I was visiting the Green House Homes at Green Hill, a continuing care facility in West Orange, N.J. Dorothy Bagli, who’s 91, showed me her room, looking out onto the garden and filled with artwork from home and photos of her grandchildren.”
Read this New York Times article in its entirety, click here.
“Things I’ll Do Differently When I’m Old” - The New York Times
 Stuart Bradford
Stuart Bradford
by Steven Petrow
“Soon after my 50th birthday, 10 years ago, I started keeping a list of ‘Things I will do/things I won’t do when I get old.’
“It was a highly judgmental, and super secret, accounting of all the things I thought my parents were doing wrong. My dad lied chronically about taking his meds. He refused to get a hearing aid, telling others to ‘up their audio’ (he had been a television producer). My mom smoked behind my back (she thought) until the day she was diagnosed with lung cancer. It was all too easy to call them out, and I recognized over and over just how awful it is to become feeble, sick and increasingly absent-minded, or worse.
“Over the next decade I accumulated many pages of dos and don’ts, even as I fretted about exactly when I’d be old enough to start following my own advice.”
Click here to continue reading this New York Times column.
“Good Friends Might Be Your Best Brain Booster As You Age” - Kaiser Health News
by Judith Graham
“Ask Edith Smith, a proud 103-year-old, about her friends, and she’ll give you an earful.

“There’s Johnetta, 101, whom she’s known for 70 years and who has Alzheimer’s disease. ‘I call her every day and just say I just say, “Hi, how are you doing?” She never knows, but she says hi back, and I tease her,’ Smith said.
“There’s Katie, 93, whom Smith met during a long teaching career with the Chicago Public Schools. ‘Every day we have a good conversation. She’s still driving and lives in her own house, and she tells me what’s going on.’
“Then there’s Rhea, 90, whom Smith visits regularly at a retirement facility. And Mary, 95, who doesn’t leave her house anymore, ‘so I fix her a basket about once a month of jelly and little things I make and send it over by cab.’ And fellow residents at Smith’s Chicago senior community, whom she recognizes with a card and a treat on their birthdays.”
You can read this Kaiser Health News article in its entirety, click here.
“How uninsured adults access health care” - Journalist’s Resource
by Chloe Reichel
“Uninsured adults use emergency rooms at similar rates to those with insurance, new research finds. Scholars at Harvard, the University of Chicago and MIT present this finding to correct what they call a ‘common misperception that the uninsured use the ED [Emergency Department] more than the insured.’
“In fact, they found that adults insured through Medicaid — public insurance for the poor — use the emergency room more than those without insurance. Looking at survey data from 2013, the researchers found that 12.2 percent of uninsured adults had visits to the emergency room compared with 13.7 percent of insured adults. Of those who had insurance, 29.3 percent of adults on Medicaid made emergency room visits. Fewer privately insured adults — 11.1 percent — went to the emergency room.
“The researchers also looked at data to categorize these emergency room visits. They found that insured and uninsured adults used the emergency room in similar ways.”
Continue reading this report at Journalist’s Resource, click here.